Type 1 Diabetes Mellitus
includes:
Important points in history
- Polyuria, thirst and polydipsia
- Polyphagia
- Weight loss
- Vomiting
- Abdominal pains
- Onset of enuresis in a previously toilet - trained child
- New presentation or acute episode in known diabetic? What is the usual insulin requirement? Any precipitating factors? Any focus for infection?
Diagnosis
Symptoms + random blood sugar (RBS) >11.1mmol/L (>200mg/dl)
Or
Fasting BS >7mmol/l (126mg/dl)
(Conversion: 1 mmol/l glucose approximately = 18 mg/dl)
In the absence of clear symptoms, diagnostic testing should be repeated on a separate day.
Other rarer types of diabetes:
- Type 2 diabetes: Usually presents in adulthood, but can present in adolescents, particularly if overweight and inactive. May be a FH. Often respond to healthy diet & weight reduction.
- Malnutrition related diabetes and fibrocalculous pancreatopathy. (can present with abdominal pain and calcification on X-ray or ultrasound.
- Neonatal diabetes (presenting in the first 6 months of life)
Treatment consists of
- Lifelong insulin dependency with multiple daily injections
- A healthy eating plan
- Regular physical activity
Diabetic Ketoacidosis
Diabetic Ketoacidosis (DKA) =
Hyperglycaemia RBS >15 or 270mg/dl + ketonuria + acidosis
(if blood gas available pH <7.3 or bicarbonate <15 mmol/l)
Important points in history & examination
- Vomiting, abdominal pain, flushed cheeks
- Ketoacidotic smell of breath
- Dehydration
- Rapid, shallow breathing (Kussmaul breathing)
- Reduced conscious level
- Abdominal rigidity - may mimic appendicitis or pancreatitis
Assess
- Severity of dehydration– usually approximately 7.5% dehydrated. Do not correct above this without consultant decision
- Level of consciousness
- Evidence of infection
Relevant Investigations
- Blood sugar - (>15mmol/l or >270 mg/dl)
- Urine Glucose high > 3-5%; Ketones high +++ or ++++
- (If available capillary blood gas & Urea and Electrolytes)
- Screen for infection i.e. Blood culture, urine dipstick, consider FBC.
Acute complications
- Cerebral oedema (& raised ICP)
- Thrombosis, haemorrhage
- Hypokalaemia (secondary to insulin) can lead to Cardiac arrest.
- Acute renal failure
Management of Diabetic Ketoacidosis
*******Correct acidosis and high blood sugars slowly *******
1. ABCCCD
Give O2 to patients with circulatory impairment or shock
2. Fluid Replacement
- Insert large IV cannula, if not possible intra-osseus access
- IV Fluids are the most important resuscitation measure. Start Normal saline or Ringer’s lactate
- Give 10mls/kg bolus 0.9% Normal saline only if shock is present (do NOT give further fluid boluses without discussing with the consultant on call)
- Fluid requirement = (Maintenance) plus (deficit)
- Write the calculation in the notes
| Child weighing 20kg on admission in shock in DKA
1 x 10 mls/kg bolus needed to correct shock = 200mls
Maintenance = 1500ml /day (1.5L)
Deficit = 20 kg x 7.5% = 1.5 L
Requirement (over 48 hours) =
Maintenance (1.5 + 1.5) + Deficit (1.5)
4.5 litres/ 48 hours = 94 mls/hr |
3. Insulin Therapy
- Insulin should be short acting, soluble (‘clear’)
- This can be given intravenously via syringe pump (preferred choice) or subcutaneously
- START INSULIN 1 HOUR AFTER STARTING IV FLUIDS
- Start IV at 0.05 units/kg/h
- Use a syringe pump - dilute 50 units short-acting [soluble] insulin eg Actrapid in 50 ml normal saline, 1 unit = 1 ml
(e.g For a 25kg child give 1.25 ml/hr =1.25 units per hour)
- Do not give an insulin bolus
- Ensure a slow drop in glycaemia <3-5mmol/l/h
- Once RBS < 15 mmol/l (250-300mg/dl) change fluid to 0.9% NaCL & 5% dextrose. Do not reduce rate of insulin (to make this fluid add 100ml of 50% glucose to every litre of 0.9% saline.)
- If blood glucose levels start to rise rather than fall consider whether need to increase rate of fluids (recalculate % dehydration) or whether need to increase insulin to 1U/kg/h
Subcutaneous insulin
- Commence 0.1u/kg SC short acting/soluble insulin. Recheck blood glucose after one hour. Repeat hourly until blood glucose is falling.
- When falling give 0.1 units/kg 1-2 hourly.
- Ensure a slow drop in glycaemia <3-5mmol/l/h
- Once RBS < 15 mmol/l (250-300mg/dl) change fluid to 0.9% NaCL & 5%
dextrose (To make this add 100ml of 50% glucose to every litre 0.9% saline.)
When to switch to maintenance insulin therapy:
Stop insulin infusion or 2 hourly SC regime when ketosis is resolving, the child is fully alert and oral fluids are tolerated without nausea or vomiting. pH should be > 7.3. The first dose of subcutaneous insulin should be given 1-2 hours before stopping insulin infusion
3. Potassium replacement
Potassium replacement is needed for every child in DKA if they are passing urine. Add KCL to IV fluids (20 mmol to each 500ml bag). If K+ <2.8 or >6, ECG monitoring advisable.
4. Ongoing management
- Monitor blood glucose levels hourly and when patient is stable every 2 hrs. Educate parents to prompt this to happen.
- Consider NGT on free drainage for child who is unconscious
- Check each urine passed for glucose and ketones as a guide to recovery
- IV fluid should be continued until the child is drinking well and able to tolerate oral feeds. The urine should be ketone free.
- Please inform the Diabetes Nurse/ team for patient educational support
5. Treatment of infection
- Infection can be a precipitant of infection. It can be difficult to exclude as the white cell count can be high due to stress and acidosis. Fever is a more reliable sign. If infection is suspected treat with broad spectrum antibiotic e.g. Ceftriaxone.
6. Cerebral oedema
- This is a rare but fatal complication of DKA. Signs include headache, vomiting, irritability, slowing heart rate and rising blood pressure, reduced conscious level, seizures. Neurological signs eg unequal pupils, posturing.
- Risk factors include: Young age, first presentation, early start of insulin, too rapid drop in glycaemia, too much iv fluid
- TREAT URGENTLY
- Exclude hypoglycaemia as a cause for change in neurological state
- Reduce the rate of fluid administration by one third
- Give mannitol 0.5-1g/kg/d over 20 minutes and repeat if there is no initial response in 30 mins to 2 hours
- Hypertonic 3% saline 5ml/kg over 30 minutes is an alternative
- Elevate the head of the bed to 30 degrees
- Consider intubation
- Consider neuro-imaging to rule out other intra-cerebral causes of neurological deterioration
7. Initial maintenance insulin requirements
once DKA has resolved and the child is drinking and eating
- Calculate the total daily dose of insulin once the child is stable. For new diabetics this is usually 0.5 - 0.75u/ kg/ day, but bear in mind their insulin requirement over the previous 24 hours. Children can have an initial 'honeymoon period' where they require less insulin.
- Initial total daily dose 0.5-0.75u/ kg/ d. Two thirds 2/3 of the total dose given before Breakfast and 1/3 before Dinner.
- At each injection 1/3rd is short acting, 2/3rd is intermediate acting.
EXAMPLE
Child weighing 36kg
For 0.5u/kg/d total daily dose of insulin = 18 units
| AM
(pre breakfast) | PM
(pre evening meal) |
| Short acting (Soluble) | 4 | 2 |
| Intermediate acting (Lente) | 8 | 4 |
Long term management of diabetes
Attend Diabetes clinic (Friday morning) once a month when glycaemic control is stable.
At each clinic review the following
1. Investigations
- Height and weight
- Fasting blood sugar
- Review of injection sites to review signs of lipodystrophy
- Foot examination for neuropathy, infections, ulcers (annually)
- Blood pressure (annually over 12 years)
- HBA1c (at least annually, ideally 3x yearly)
- Urine dipstick. If proteinuria check creatinine & urea. If persistent albuminuria consider ACE inhibitors & Renal Review
- Ophthalmology review (annually)
2. Assess for hypoglycaemic awareness and hyperglycaemic symptoms
- Nocturia? Thirsty? A good guide of blood sugar control is how many times the child has to pass urine over night.
- Hypo symptoms: sweating trembling, tachycardia, drowsiness, confusion
- Treatment: Glucose in form of refined sugars e.g. sobo
3. Blood Glucose monitoring
- Check whether have glucometer and ensure provided with a number of sticks each clinic
- Review blood glucose monitoring booklet
- Patterns of blood glucose levels (BGLs) are more important than a single BGL
- Should test strips be scarce, it is best to test at different times of the day a few days a
week rather than the same time each day. If possible, test regularly before and two
hours after breakfast and all other meals, and periodically overnight at 3am (checking
for hypoglycaemia).
Recommended target blood sugar range:
Before meals: 4-7mmol (72-126mg/dl)
After meals: 5-10mmol/l (90-180mg/dl)
At bedtime: 10mmol (180mg/dl)
At 3am: 5-8mmol/l (90-144 mgl/dl)
Hypoglycaemia = blood glucose <3.9 mmol/l (70mg/dl)
Ongoing insulin requirements
- Pre-pubertal children (outside the partial remission phase) usually require 0.7-1.0 U/kg/day
- During puberty, requirements may rise above 1 and even up to 2 U/kg/day
- In any child requiring over 1.5 U/kg/d consider poor treatment compliance as a strong possibility. Consider admission
to Medical Bay for 2 days to review regime. (On the day 1 of admission the nurses should administer the insulin and check
RBS’s 4 hourly. Check injection technique, injection sites and diet)
- The "correct" dose of insulin is that which achieves the best attainable glycaemic control, without causing obvious
hypoglycaemia, and resulting in normal growth and development.
Insulin adjustment
Review blood sugar booklet, HBA1c & symptoms to guide alternation of regime. DO NOT INCREASE INSULIN BASED ON AN ISOLATED HIGH BGL IN CLINIC as this may be a rebound from hypoglycaemia in the middle of the night (Somogyi effect.)
- If a pre-meal BGL is always high, the preceding dose of intermediate acting insulin (lente) may be insufficient.
- If the pre-meal BGL is always low, the previous dose of intermediate insulin (lente) may be too high.
- If a pre-meal BGL is sometimes very high and at other times very low, either insulin, food or exercise are not consistent and should be reviewed.
- If the BGL 2 hours after the meal is too high, the previous meal dose of shortacting (regular) insulin may be too low.
- If the BGL 2 hours post-meal is too low, the previous meal dose of shortacting (regular) insulin may be too high.
- NB the level of blood glucose can rise in the early morning, so care should be taken if increasing the evening intermediate dose as nocturnal hypoglycaemia may go unnoticed which can be dangerous.
HBA1c
HBA1c (glycated haemoglobin) provides information about the average blood glucose levels over the past 2-3 months. The target HbA1c for all age-groups is < than 7.5%. Check HBA1c at least once yearly (ideally 3 times yearly)
Education
Patient education is the cornerstone of good glycaemic control
Diet
- Importance of regular meals
- Avoid refined sugars e.g. Sobo, coke, fanta, any sugar in tea, cakes and biscuits
- Encourage complex carbohydrates e.g. cereals and a high fibre diet
- Encourage the whole family to adopt this healthy diet
Insulin
- Keep in a cool place (ideally a fridge; if unavailable place insulin in a small clay pot, then place small pot into a larger pot containing water - evaporation of the water will cool the inner pot)
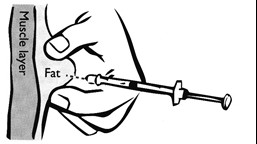
- Rotate injection sites to prevent erratic insulin absorption from lipodystrophy. Use the stomach, thighs, buttocks and upper arms
Hypoglycaemia awareness
- Hypo symptoms: sweating trembling, tachycardia, drowsiness, confusion
- Treatment: Glucose in form of refined sugars e.g. 200ml (half a cup) sweet juice eg sobo followed by 10-15g of a slow acting carbohydrate eg Nsima
Sick day rules
- Increase fluid intake
- Do not stop insulin even if unable to eat
- Seek medical attention if child is unable to drink or breathing fast or drowsy
Exercise
Monitor for complications
- Poor glycaemic control may lead to growth failure & puberty delay
- Retinopathy resulting in visual loss
- Diabetic nephropathy causing hypertension and renal impairment
- Neuropathy causing pain, parathesia, muscle weakness, autonomic dysfunction
- Macrovascular disease causing cardiac disease, stroke and peripheral vascular disease with limb loss, impotence
- Hypothyroidism can develop
Consider anti-hypertensives if blood pressure is consistently > 95th centile or > 130/80 mmHg Hypertension
Reference:
http://www.idf.org/sites/default/files/Diabetes-in-Childhood-and-Adolescence-
Guidelines.pdf
- British Society of Paediatric Endocrinology DKA Guidelines 2015
http://www.bsped.org.uk/clinical/docs/DKAguideline.pdf
